The DIDA condemns improper charges to patients
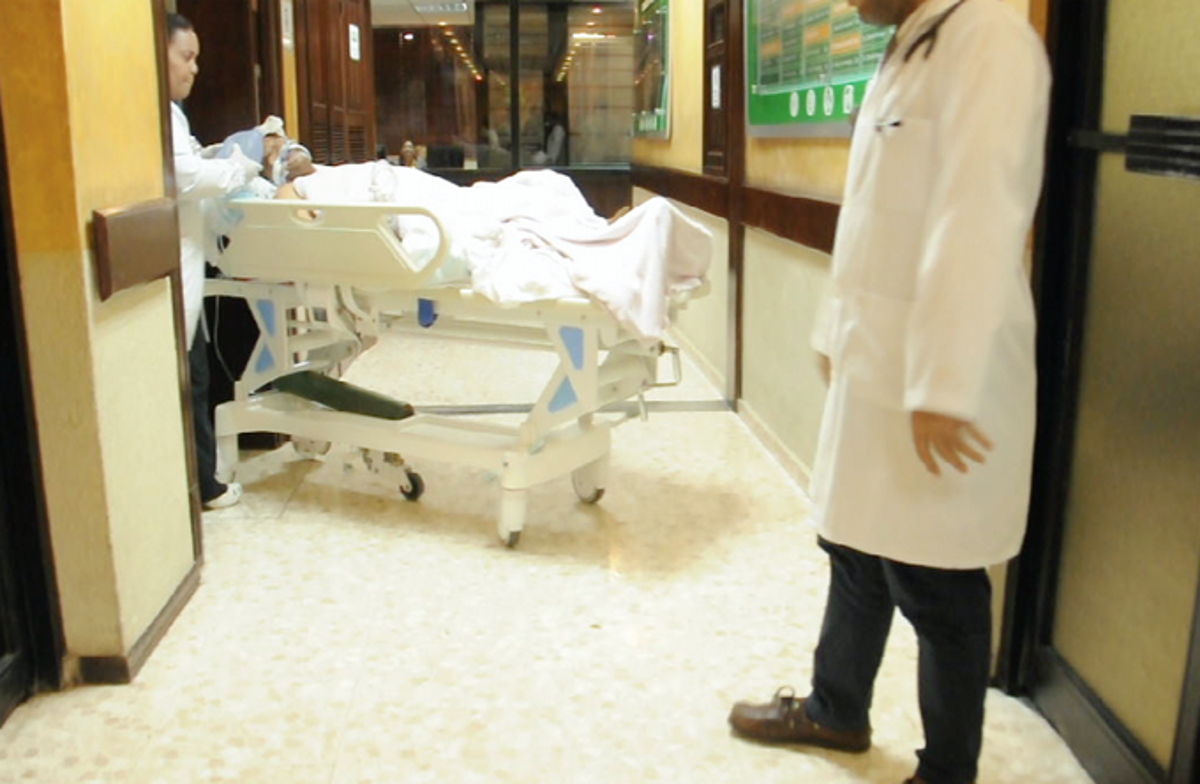
Ready to defend. In the current administration, they have dealt with 128 cases of complaints about the improper collection of deposits or payments above what is established.
The General Directorate of Information and Defense of Social Security Affiliates (DIDA) yesterday joined the debate generated by complaints from patients about the practice of demanding the payment of advances and deposits for admission to health centers and about the treatment little humanized that sometimes they receive.
The director of the DIDA, Carolina Serrata Méndez, responded to this by warning Health Service Providers (PSS) not to make improper charges to social security affiliates.
In addition, he called on the Health Risk Administrators (ARS) to comply with the provisions that establish the exclusion from their network of doctors and health service providers who repeatedly engage in this practice that is harmful to the health and pockets of members.
In a press release, the director of the DIDA reminds providers that they must guarantee the medical care contemplated in the legal regulations and the resolutions issued by the Superintendency of Health and Occupational Risks (SISALRIL).
Director asks for respect.
Serrata Méndez called on the Health Risk Administrators (ARS) to comply with SISALRIL resolutions 156-2008 and 175-2009, which order the exclusion from their network of medical centers and health service providers that repeatedly incur in this harmful practice to the health and the pocket of those affiliated to the Dominican Social Security System (SDSS).
He said that “according to the statistics of the DIDA, during our management we have received 128 cases for improper charges, for deposit or payments above the established, of which we have closed 136.”
Solutions to complaints
He explained that these numbers of closed cases exceed the number received in his management, since cases inherited from the previous administration have been resolved, of which 113 claims have been resolved in favor of those affiliated with social security, ” evidence that the claim that is formalized in the DIDA is determined, as appropriate.
Rights of affiliates
The official reiterated to the affiliates that if they are affected by the improper charges, they have the right to a refund of the amount paid by simply presenting an invoice or receipt of payment, first, to their ARS and in case of not being compensated satisfactorily, file your claim with the DIDA.
Data
The procedure
The director of the DIDA, Carolina Serrata Méndez, explained that the procedure to follow in the event of an improper charge is to notify your ARS from the same health service provider immediately and if you made the payment, you have a period of 60 days to claim the improper charge in emergency care or 90 days for improper charge in hospitalization by the Health Service Providers (PSS).